The Vagus Nerve & The Pelvic Floor: The Emotional-Structural Bridge
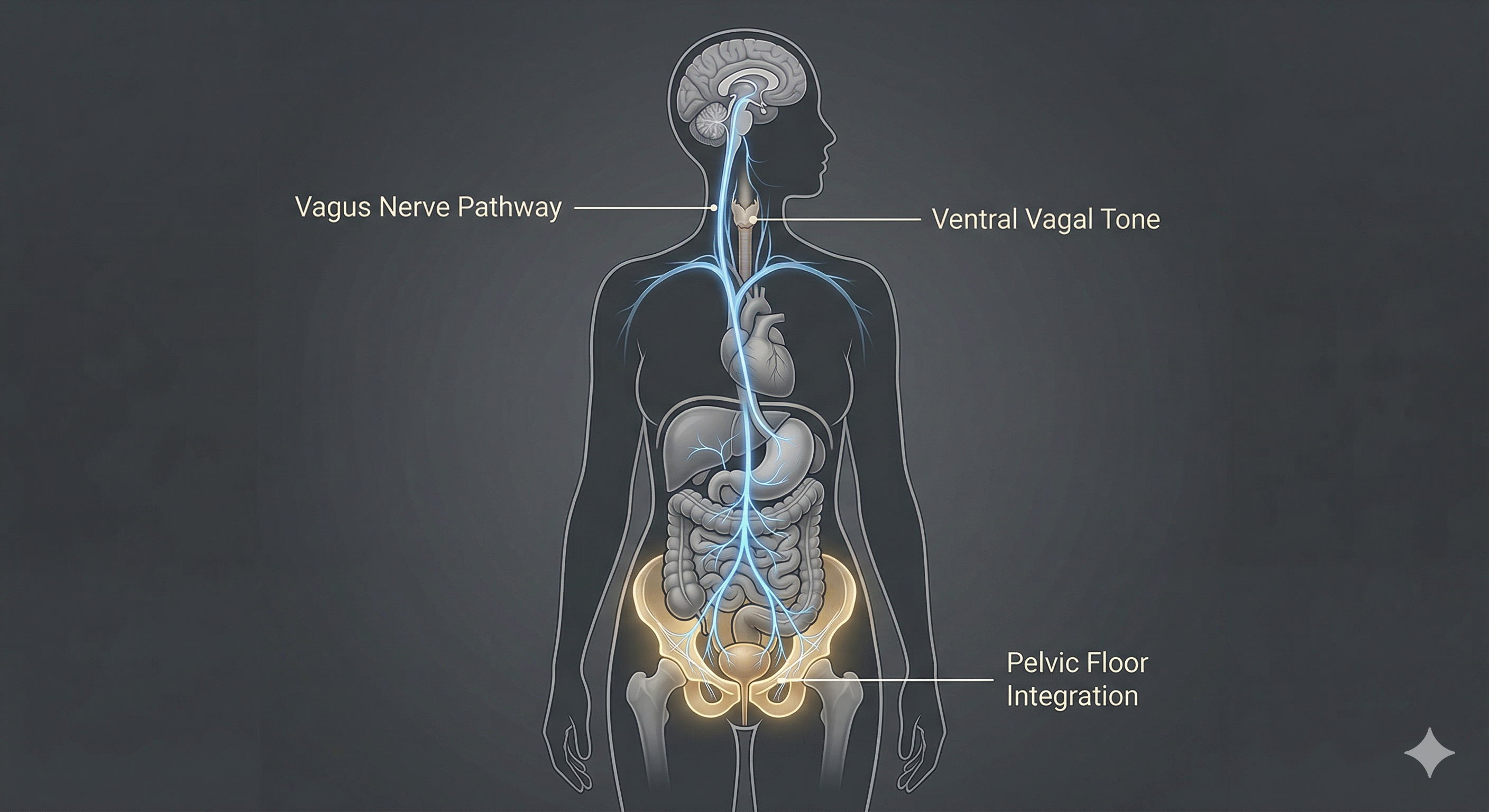
In the Second Spring, we often treat the pelvic floor as a purely mechanical structure—a group of muscles to be "strengthened." However, clinical neurology reveals a much deeper story: the pelvic bowl is the southern anchor of the Vagus Nerve, the primary conductor of our "Rest and Digest" system.
The Polyvagal Connection
The Vagus Nerve (Cranial Nerve X) is the longest nerve in the autonomic nervous system. It wanders from the brainstem through the heart and lungs, finally terminating in the deep viscera of the pelvis. When we are in a state of chronic "High Alert" (Sympathetic dominance), the Vagus nerve sends a signal of contraction to the pelvic floor. This is why "stress" often manifests as pelvic tension or urgency—it is a neurological reflex, not just a muscular one.
Diaphragmatic Synergy: The Piston Effect
The respiratory diaphragm and the pelvic floor work together like a synchronized piston. When you inhale deeply, your diaphragm drops, and your pelvic floor should naturally lengthen and soften. In the Spring Phase, shallow "chest breathing" becomes common due to cortisol shifts, breaking this synergy. By restoring Ventral Vagal Tone through slow, nasal breathing, we manually reset the tension held in the pelvic bowl.
The Sanctuary Protocol: The Vagal Reset
The Hum Ritual: The Vagus nerve passes right by the vocal cords. Gentle humming during an exhale (Brahmari Pranayama) creates a vibration that stimulates the nerve, sending an immediate "safety" signal to the pelvic floor. Try 5 minutes of low-pitched humming before bed to down-regulate the entire system.
Structural Release vs. Strengthening
For many women over 50, the issue isn't a "weak" pelvic floor, but a "hypertonic" (overly tight) one. Constant Vagal "noise" keeps these muscles in a state of guarded contraction. Before we strengthen, we must release. Using specific hand mudras or restorative yoga postures like "Happy Baby" allows the Vagus nerve to communicate safety to the tissues, allowing for true functional resilience.
Physiological FAQs: Vagus & Pelvis
Can Vagus nerve stimulation help with bladder urgency?
Yes. Bladder urgency is often a sign of an overactive nervous system. By increasing Vagal tone through breathwork and vocalization, you soothe the "urgency" signals being sent to the brain, leading to better bladder control.
<div>
<h4 style="color: #4361EE; font-weight: 800; font-size: 1.1rem; margin-bottom: 0.5rem;">What is "Ventral Vagal Tone"?</h4>
<p style="color: #6b708d; line-height: 1.8;">Ventral Vagal Tone refers to the state of the nervous system where we feel safe, connected, and relaxed. This is the optimal state for healing, digestion, and pelvic floor flexibility.</p>
</div>
Frequently Asked Questions
Can Vagus nerve stimulation help with bladder urgency?
Yes. Urgency is often linked to nervous system overactivity. Stimulating the Vagus nerve sends 'safety' signals that calm the bladder reflex.
What is 'Ventral Vagal Tone'?
It is the state of the nervous system associated with safety and relaxation, allowing the body to properly repair tissues and regulate pelvic tension.
Weekly Physiological Briefings
Clinical insights and nervous system rituals delivered once a week. No noise. Just wisdom.
Want this protocol molded to your specific rhythm?
Talk to the Sanctuary Guide to adjust these insights for your bio-individual needs.